Empowering Ehlers-Danlos Syndrome Management: Integrating Carnivore Diet, Regenerative Therapies, and Nutritional Science Myths
Understanding the Complexities of Ehlers-Danlos Syndrome
For those living with Ehlers-Danlos Syndrome (EDS), each day presents unique challenges that extend beyond physical symptoms. EDS, a group of hereditary disorders that primarily affect connective tissues, varies widely in its manifestation but often includes chronic pain, joint dislocations, and a propensity for bruising. However, one of the lesser-known complications associated with EDS is Cranial Cervical Instability (CCI), a condition where the ligaments in the neck are too lax, leading to compression of the brainstem or spinal cord.
Diagnosing CCI can be particularly thorny due to its blend of neurological and musculoskeletal symptoms, which often overlap with other conditions. Patients report a range of experiences from severe headaches and dizziness to cognitive difficulties and emotional lability. This complexity requires a comprehensive, interdisciplinary approach to management, highlighting the importance of patient advocacy in securing proper diagnostic evaluations.

For those living with EDS and CCI, self-awareness and education are vital. Understanding the symptoms helps in managing emotional impacts, as these conditions are often misunderstood even within the medical community. Emotional regulation becomes an essential aspect of daily life, requiring not only medical interventions but also psychological resilience and support strategies.
The Promise of Regenerative Therapies for Joint and Ligament Stability
Regenerative therapies have emerged as a beacon of hope for individuals with EDS dealing with ligament laxity. Procedures like Platelet-Rich Plasma (PRP) and prolotherapy are gaining traction for their innovative approach to promoting tissue repair and stability. These therapies utilize biological components to stimulate the body’s natural healing mechanisms, thereby addressing the root cause of instability.
PRP therapy involves the use of platelets concentrated from the patient’s own blood. These platelets are rich in growth factors, which, when injected into damaged ligaments, can accelerate healing. Meanwhile, prolotherapy employs a slightly different method—injecting an irritant solution to stimulate the body’s healing response, potentially strengthening the tissue over time.
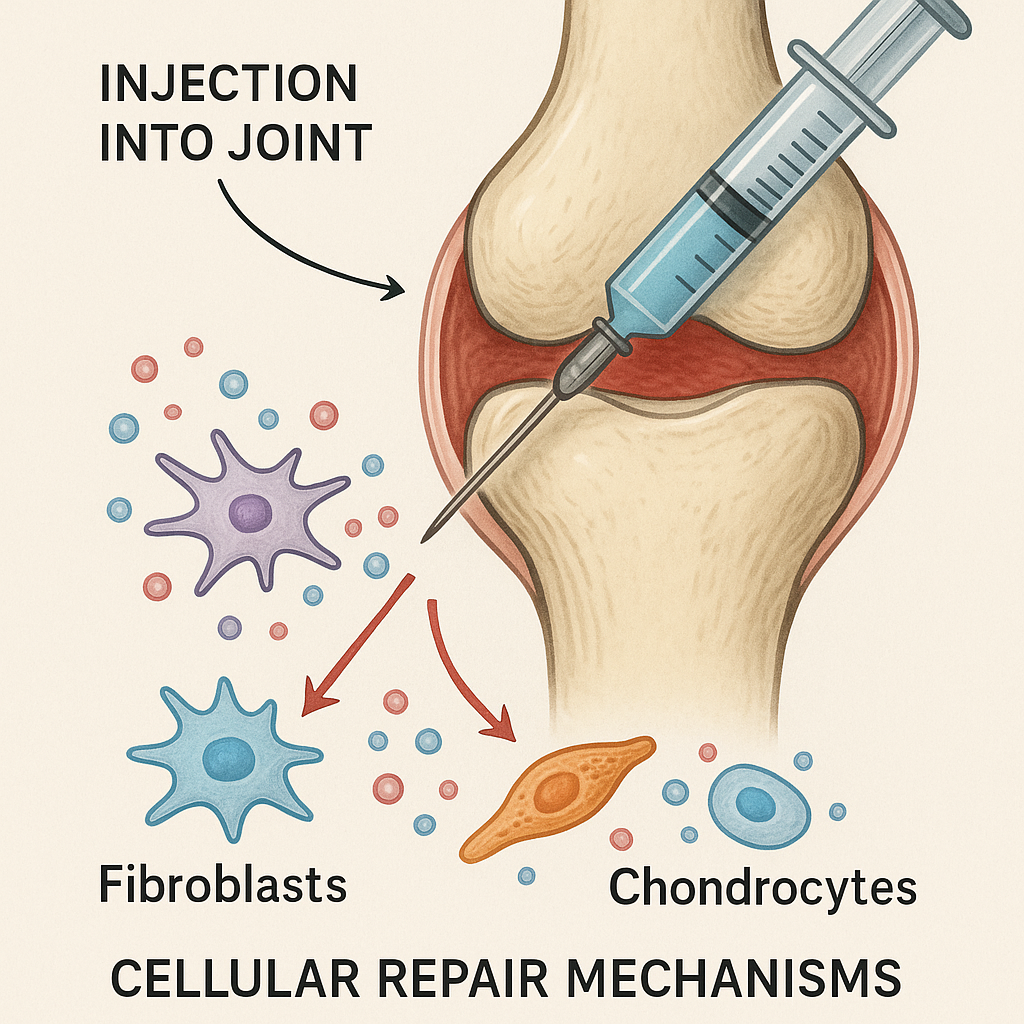
Studies suggest promising results, with many patients reporting improved joint stability and reduced pain. However, outcomes can vary based on individual conditions and the chronicity of the symptoms. As with any treatment, ongoing research and personalized treatment plans are crucial in maximizing the benefits of regenerative therapies.
Re-evaluating Nutrition: The Carnivore Diet’s Role in Connective Tissue Health
Within the realm of nutritional interventions, the carnivore diet is gathering interest for its potential to alleviate symptoms linked to connective tissue disorders. A diet that focuses exclusively on animal-based products, the carnivore diet argues for a radical departure from conventional dietary recommendations, which often emphasize carbohydrates and plant-based foods.
Advocates suggest that by eliminating foods known to trigger inflammation, the carnivore diet may offer relief from some symptoms associated with EDS. The high collagen intake from animal sources might directly support tissue repair, while also simplifying dietary intake for those sensitive to various food groups.
However, critical evaluation of nutritional myths is necessary. The ongoing debate about dietary fiber suggests that while traditionally deemed essential, its necessity could be overstated, particularly in specific metabolic health contexts. Similarly, the understanding of cholesterol is evolving, with newer research disentangling its link to heart disease from previous misconceptions.
Biochemistry and Cellular Insights into Inflammation and Repair
Exploring the biochemistry of diet’s impact on chronic conditions illuminates how dietary choices may influence inflammation and tissue repair at the cellular level. In EDS management, understanding these pathways is particularly pertinent. Inflammation, a common component of chronic pain, may be mitigated through dietary strategies that prioritize anti-inflammatory properties inherent in animal-based nutrition.
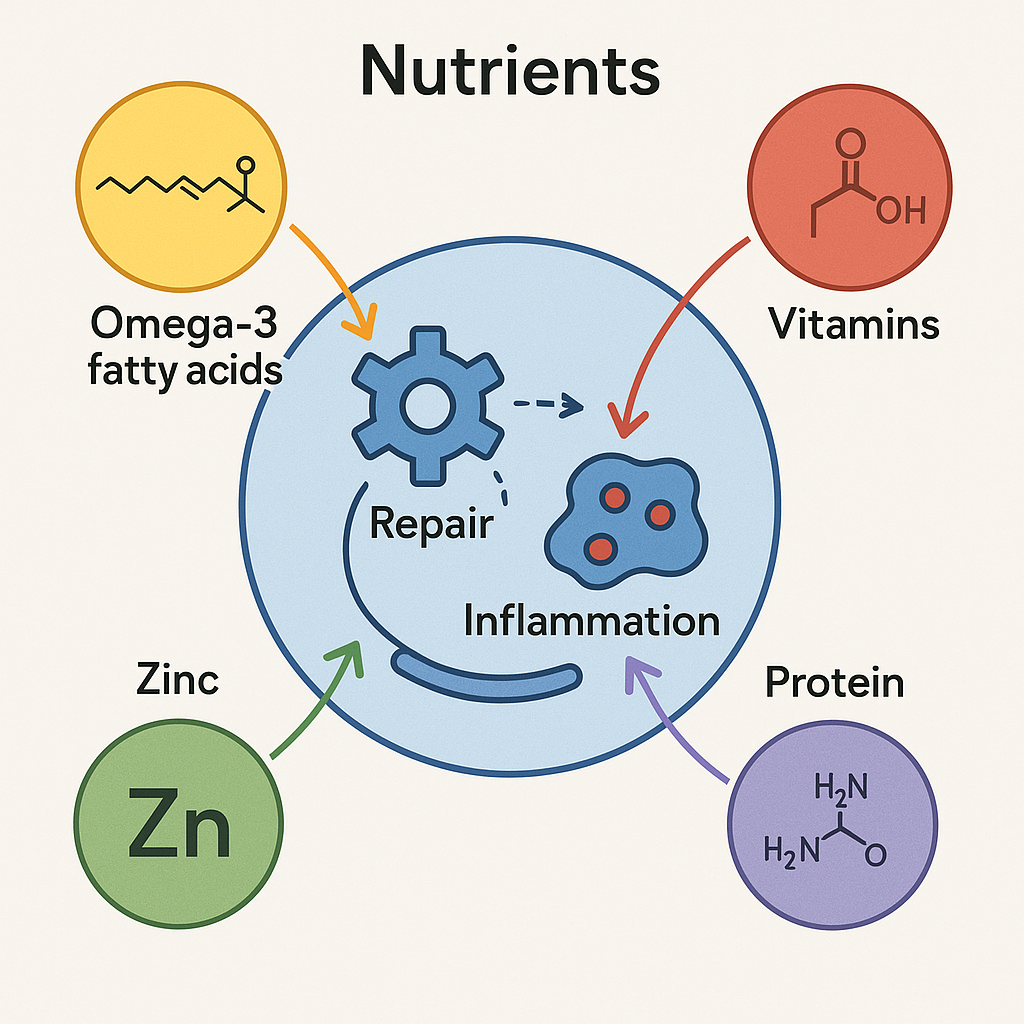
At the cellular level, nutrients play a pivotal role in maintaining vascular health. Essential fats and proteins found in animal products contribute to the repair and stability of tissues, important for those dealing with vascular forms of EDS. By diving into the molecular intricacies of how nutrition supports cellular processes, patients and healthcare providers together can pave a new way in chronic illness management.
Empowering Through Education and Advocacy
In the face of chronic illnesses, self-education and patient advocacy become empowering tools for navigating an often confusing healthcare landscape. Access to reliable information allows individuals to make informed decisions about treatment options and lifestyle adjustments. Utilizing resources such as online courses in biology and nutrition can demystify complex concepts, fostering a deeper understanding of one’s own health.
Moreover, maintaining open dialogue with healthcare providers and expressing one’s needs and preferences are crucial steps toward receiving appropriate care. Establishing a collaborative relationship can lead to more personalized treatment strategies and better outcomes.

Understanding the psychological landscape of chronic illness is also vital. Emotional support and community connections bolster resilience, reducing the isolation often felt by those with misunderstood conditions. Thus, integrating psychological well-being into treatment plans enables a holistic approach to managing EDS and similar disorders.
Integrating Strategies for Improved Quality of Life
While Ehlers-Danlos Syndrome presents formidable challenges, emerging strategies in nutrition and regenerative medicine offer promising avenues for empowerment. By critically engaging with scientific advancements and discarding outdated nutritional myths, individuals can assert control over their health journeys.
Through comprehensive approaches that combine evidence-based therapies with nutritional insights, improving quality of life becomes an attainable goal. Empowerment through education, coupled with supportive healthcare collaborations, places patients at the forefront of their healing journey, inspiring hope and fostering resilience amidst adversity.



